Understanding Knee Pain: A Common Concern for Canadians
Knee pain can affect people of many ages in Canada, from active teens to older adults managing day-to-day mobility. Because the knee carries body weight and supports twisting, bending, and impact, it is vulnerable to overuse and injury. Understanding common causes and practical management options can help you make informed choices about care.
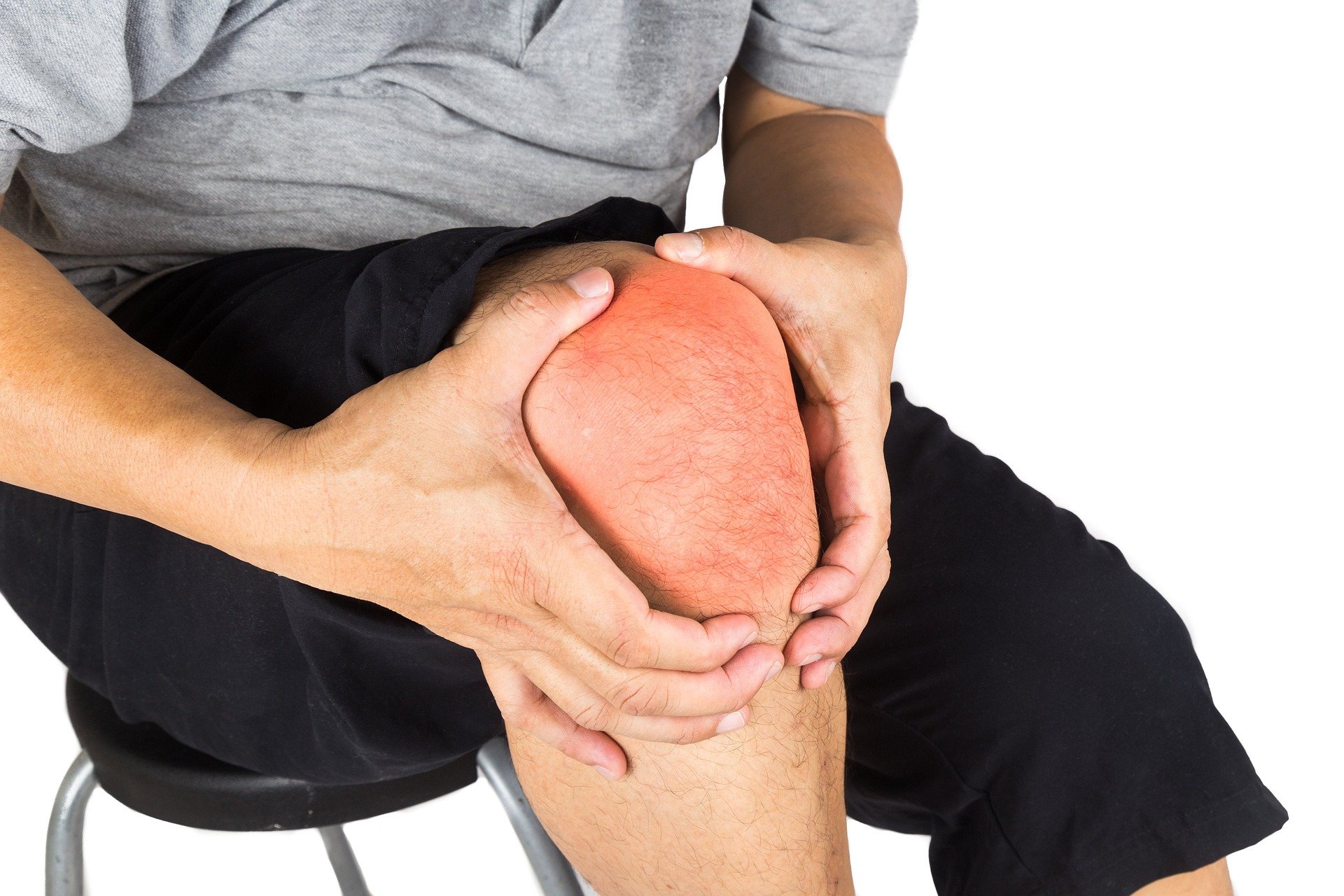
Knee pain is one of the most frequent reasons people change how they move, exercise, work, or handle everyday tasks like stairs and getting in and out of a car. In Canada, it often shows up alongside busy schedules, recreational sports, winter slips, and long periods of sitting or standing. This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
What Is Knee Pain?
Knee pain is discomfort felt in or around the knee joint, which includes bones, cartilage, ligaments, tendons, and surrounding muscles. Pain can be sharp after a sudden twist or fall, or it can be dull and achy over months. Some people notice stiffness in the morning, swelling after activity, grinding sensations, or a feeling that the knee may “give way.” The location matters: pain at the front of the knee often differs from pain along the inner or outer joint line, or behind the knee.
Common Causes of Knee Pain
Common causes range from overuse to structural injury and inflammatory conditions. Osteoarthritis is a frequent contributor, especially with age or prior injury, and may cause stiffness and pain with walking or stairs. Meniscus tears can occur with twisting or gradually with wear, and may cause catching or joint-line tenderness. Ligament sprains (such as ACL or MCL) are more common after sports or falls. Patellofemoral pain, tendinopathy, and bursitis can develop from training changes, repetitive kneeling, or muscle imbalances.
Non-Surgical Management Approaches
Many cases improve with conservative care focused on function, not just pain relief. Activity modification can reduce aggravating movements while you stay active through lower-impact options (cycling, swimming, or walking intervals). A physiotherapy program often targets hip and thigh strength, balance, and joint mechanics to reduce load on sensitive tissues. Weight management can lower knee joint stress for some people. Pain strategies may include ice or heat, short-term use of over-the-counter pain relievers when appropriate, and supportive footwear or braces, depending on the problem.
When Further Care May Be Considered
Further assessment may be appropriate if pain persists beyond a few weeks, worsens, or limits daily activities despite self-care. Immediate medical attention is important after a significant injury (especially with a “pop,” rapid swelling, or inability to bear weight) or if there are signs such as fever, redness and heat around the joint, severe night pain, or a swollen calf. A clinician may consider imaging based on symptoms and exam findings. Injections or specialist referral (for example, to sports medicine, rheumatology, or orthopedics) may be discussed when conservative steps are not enough.
In Canada, care often starts with a family doctor, nurse practitioner, walk-in clinic, or a physiotherapist (depending on the province and your insurance coverage). Examples of widely available organizations and networks that may help with assessment, rehabilitation, or next-step navigation include:
| Provider Name | Services Offered | Key Features/Benefits |
|---|---|---|
| Lifemark Health Group | Physiotherapy, rehab, exercise therapy | Multi-location clinic network in several provinces |
| CBI Health | Physiotherapy, rehab, pain programs | Broad clinic footprint and multidisciplinary services |
| Myodetox | Physiotherapy, movement-focused rehab | Clinic-based care with emphasis on active treatment |
| Maple | Virtual medical visits | Telemedicine access for medical guidance and referrals |
Living With Knee Pain
Living well with knee pain often means combining symptom control with a clear plan to build capacity over time. Tracking what triggers symptoms (distance walked, hills, deep squats, kneeling) can help you pace activity and avoid flare-ups. Gradual strengthening and consistent mobility work can improve confidence and reduce re-injury risk. For work and home, small adjustments such as using handrails, changing how you lift, or breaking tasks into shorter bouts can reduce load. If pain affects mood or sleep, addressing stress and recovery habits can also support progress.
Knee pain is common, but it is not one-size-fits-all: the cause, location, and pattern of symptoms influence which strategies help most. Many people improve with well-chosen non-surgical approaches that emphasize strength, movement quality, and sensible activity progression. When symptoms are severe, persistent, or linked to warning signs, timely medical assessment can clarify the diagnosis and guide the safest next steps.